Calculating DALYs: UVR and skin cancer
- The text on this page is taken from an equivalent page of the IEHIAS-project.
As part of the EU-funded INTARESE project, which contributed to the development of this Toolbox, a case study was conducted to assess health impacts due to skin cancer associated with ultra-violet radiation (UVR) under different climate change scenarios.
Health impacts were assessed in terms of disability-adjusted life years (DALYs).
The DALY is a health gap measure that combines both time lost due to premature mortality and non-fatal conditions. The DALY combines in one measure the time lived with disability and the time lost due to premature mortality. DALYs for a disease or health condition are calculated as the sum of the years of life lost due to premature mortality (YLL) in the population and the 'years lived with disability' (YLD) for incident cases of the health condition.
- YLL: The YLL is calculated by combining the mortality due to the health condition with the expected life expectancy for each age(group).The WHO’s Global Burden of Disease (GBD) study (WHO 2008; Mathers et al 2001) used the same life expectancy ‘ideal’ standard for all population subgroups, whether or not their current life expectancy is lower than that of other groups. To define this Standard Expected Years of Life Lost (SEYLL), the highest life expectancy observed for any nation (i.e. the 82.5 years life expectancy of women in Japan) was chosen. The standard expectations are therefore based on a model life table, namely Coale and Demeny West level 26, which have a life expectancy at birth for females of 82.5 years. Following the WHO GBD-study (WHO 2008) and the 2001 Victorian Burden of Disease study (DHS 2005), WP3.7-UVR uses this standard life expectancy for calculating YLL.
- YLD: Years lived with disability (YLD) are the disability component of DALYs that describe the time spent with a disease or injury for a specified duration, adjusted for severity. The YLD uses explicit preference weights for health states. Hence, the severity of a diseases is indicated with disability weights (DW), expressed on a scale from zero to one, with zero being full health/no disability and one representing death.
As part of the assessment of UVR and skin cancer, data on skin cancer incidence and mortality (for the baseline, SRES-B1 2030 and SRES-A2 2030 scenarios) were translated into DALYs.
| DALY = YLL + YLD
YLL = years of life lost due to premature mortality YLD = years lived with disability |
| YLL= N x L
N= Number of deaths; L= life expectancy at age of death (in years) |
| YLD = I x DW x L
I= incident cases; L= Average duration of disability (years); DW= Disease weight |
Details of the calculation are given in the worked example in the attached spreadsheet.
Explanation of the method
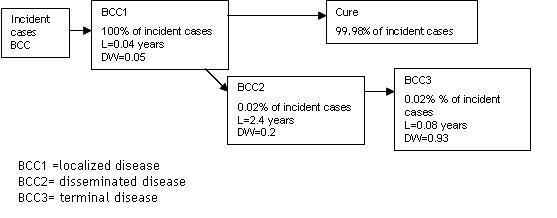
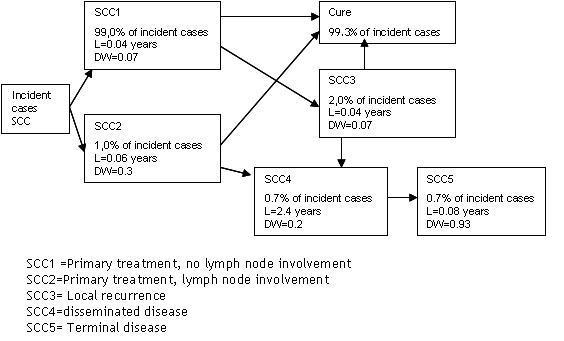
UVR:DALY calculations for Squamous Cell Carcinoma (SCC) and Basal Cell Carcinoma (BCC).
The modelled SCC and BCC incidence and mortality (for the baseline, SRES-B1 2030 and SRES-A2 2030 scenarios) were translated into DALYs. For this DALY calculation spreadsheets were developed in Excel.
These spreadsheets build on the following templates/studies:
- Disease models derived from the WHO UVR-BoD-study by Lucas et al (2006). See figures below.
- WHO standard life tables:e(a) (life expectancy at age a), West level 26.
- The WHO Global Burden of Disease Study (BoD) DALY calculations template worksheet
DW- disease weights/ L- duration.
UVR: DALY calculations for malignant melanoma (CMM)
The modelled melanoma incidence and mortality (for the baseline, SRES-B1 2030 and SRES-A2 2030 scenarios) were likjewise translated into DALYs, again using DALY calculation spreadsheets (in Excel). These built on the following templates/studies:
- Disease models derived from the 2001 Victorian Burden of Disease (BoD) study (DHS 2005). See the YLD excel worksheet for cancers, including melanoma. See Figure below.
- Note: disability weights adapted from the Dutch study (Stouthard et al 1997).
- WHO standard life tables:e(a) (life expectancy at age a), West level 26.
- The WHO Global Burden of Disease Study (BoD) DALY calculations template worksheet.
See also the example spreadsheet (.xls) appended.
[[Image:CMM_disease_model_iehias.JPG
DW- disease weights/ L- duration.
DALY calculations: WP3.7-UVR sensitivity analyses
In addition, Table 1 provides an overview of the standard DALY model setting and alternatives model settings applied in the sensitivity analyses for the UVR case study. Box 1 provides information about applying age-weight and discounting to DALY calculations, as well as adjusting for co-morbidity.
| DALY calculations standard setting: uniform age weights; no discounting; no adjustment of disease weights for co-morbidity |
|
* For 2030 calculations, discounting only calculates the net present value in 2030.
| Age weights
The GBD-study (Murray and Lopez,1996, WHO 2008) applied age weights that gave higher weight to a year of life in young and mid adult years, and lower weight to a year of life at very young and older years (non-uniform age-weighing). This choice was based on a number of studies that have indicated there is a broad social preference to value a year lived by a young adult more highly than a year lived by a young child or at older ages. Some have argued that age weighting is unacceptable on equity grounds and every year of life is of equal value, while others that age weights are not in themselves inequitable, because everyone potentially lives through every age, and that they do reflect legitimate societal priorities. Hence, the age weights are the most controversial value choice built into the DALY. Not all studies agree that the youngest and oldest ages should be given less weight; nor do they agree on the relative magnitude of the differences. The 2001 Victorian study (DHS 2005) and the 1999 Australian study (Mathers et al 1999) do not use age weights. See also: Mathers et. al (2001) National burden of disease; a practical guide. Geneva: WHO. Discounting The GBD-study (Murray and Lopes, 1996; WHO 2008) applied a 3% time discount rate to years of life lost in the future to estimate the net present value of years of life lost. A number of people have argued that discounting should not be applied to future health gains or losses and discounting is rarely used by epidemiologists and demographers for summary health measures. Discounting has a profound effect on the estimated size of benefits. See also: Mathers et. al (2001) National burden of disease; a practical guide. Geneva: WHO. Adjusting for co-morbidity The GBD did not attempt to deal with the effects of co-morbidities on DW estimates for individual diseases. The Australian projects (DHS, 2005; Mathers et al1999) adjust DW estimates for co-morbidities between mental disorders, between congenital malformations and between physical disorders at older ages. See also: [1] See also |